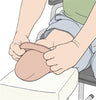
Common Skin Issues for Above Knee Amputees
Skin Issues
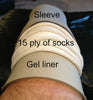
A variety of skin complications can occur around a residual limb. Many of these are preventable with diligent limb inspection and early treatment; and therefore should be brought to the attention of a physician when first noticed. The first of these skin problems is skin abrasion or breakdown, which may be attributable to inadequate sensation or blood supply to the residual limb and the inability to tolerate the pressure of a prosthesis. The prosthesis itself may not be fitted properly or may have been worn for too long; both conditions cause blisters from too much motion between the residual limb and the prosthesis. To reduce this friction, wear a nylon sheath or increase the ply (thickness) of socks worn over the residual limb. A better solution is getting the prosthesis modified to fit better. Both abrasions and blisters should be treated aggressively. Left untreated, they can result in serious infections.
The residual lower limb can also develop an unpleasant odor especially if exposed to excessive sweat and bacteria. Silicone sockets can often be a culprit since they retain moisture. Typically, this odor can be controlled by cleaning the residual limb, well but if excessive sweating is the underlying problem, then an antiperspirant can be used. Allowing the limb to be exposed to air on a regular basis will also help evaporate any moisture from the limb, so excessive wearing times should be minimized.
Other skin conditions can result from being exposed to an irritant. Contact Dermatitis will be felt as an itching, burning sensation at the site of irritation. If the skin breaks down as a result of this condition, infection can occur, causing significant problems. The cause of the irritant can be the detergent you use or a socket liner. Topical antihistamines or steroid creams may help these problems but should only be tried after consulting with one’s physician.
Verrucous hyperplasia is a skin condition caused by an ill-fitting socket. A tight socket chokes the residual limb, trapping blood at the end of the residual limb. Over time, this pooling of blood results in the formation of thick, raised, itchy and often painful tissue over the end of the residual limb that looks very much like a large wart. Left untreated, this warty skin breaks down leading to an infection. It is important, therefore, that as soon as “choking” or improper fitting is detected or tightness felt in the residual limb, the prosthesis should be modified to prevent this problem.
Epidermal cysts form when a pore gets clogged and debris gets trapped within the skin tissue of the residual limb. The most common location for these lesions is behind the knee but they can be formed on either an upper or lower residual limb. They can also vary in size from a small pea up to the size of a golf ball. Treatment requires drainage or injection of a steroid like medication to help shrink the tissue. Usually if the prosthesis is adjusted, the condition does not recur.
Related Articles:
- Alcohol & Skin Care: The Facts
- Do I have a skin disorder?
- How-to create a prosthetic skin care routine?
- How do amputees deal with friction?
- How Does Your Skin Work?
- Ingredients To Avoid
- Know Your Skin Type
- Parabens: Are they really a problem?
- The DOs and DON'Ts of Skin Care
- Why are fragrance free products best?
- Why do some skincare products cause a negative reaction?
- Your Residual Limb Deserves Some TLC
- 15 Skin Problems Amputees Experience & How to Solve Them