Using Micro-Fragmented Adipose Therapy to Treat Chronic Prosthesis-Related Ulcers
Managing ulcers related to prosthesis use on residual limbs has always been challenging in wound care and rehabilitation. A newly formed prosthetic limb requires several adjustments to fit properly, and patients’ bodies change over time. As a result, physiatrists often come across patients with pressure ulcers related to their prostheses.
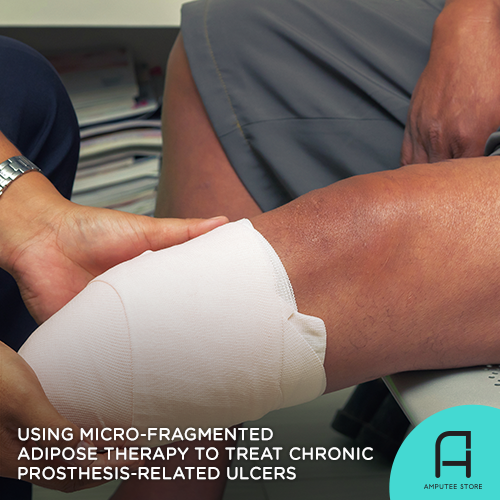
Patients who have undergone lower-limb amputation usually experience 65% more dermatologic issues than those who haven't experienced limb loss. Furthermore, approximately 75% of lower-limb prostheses patients experience skin problems. This is mainly due to increased humidity, prolonged moist contact, and high shear forces within the prosthetic limb. These factors contribute to skin tissue breakdown, leading to ulceration.
Prosthesis-related residual limb ulcers often negatively impact patients’ daily function and quality of life. Therefore, solving this issue is of the utmost importance.
Managing prosthesis-related ulcers
When residual limb ulcers occur due to prosthesis use, the usual management method is to stop using the prosthetic limb for some weeks. However, not using the prosthesis can also negatively affect the user, such as a higher risk of falls, decreased ability to walk, weight gain, psychological stress, and financial issues.
Aside from resting, doctors can treat these ulcers with wound dressings, adjusting the prosthetic socket, negative pressure wound therapy, surgical debridement, bioengineered skin substitutes, and hyperbaric oxygen therapy.
The patient
A study was conducted to investigate the effectiveness of micro-fragmented adipose tissue therapy as a potential method for managing ulcers. The case of a 56-year-old male was considered, who had a history of left below-knee amputation, lumbar spinal stenosis, and left total knee replacement. The patient had a non-healing stage 2 prosthesis-related residual limb ulcer for three years, which did not respond to various treatments such as discontinuing the prosthesis, adjusting the prosthetic socket, using silicone socks, and bioengineered skin grafts.
In June 2020, the patient experienced increased pain associated with prosthetic limb use after a hike, and the ulcer on their residual limb worsened. The patient decided to explore non-surgical options and opted for micro-fragmented adipose tissue therapy over a skin autograft.
What is micro-fragmented adipose therapy?
Micro-fragmented adipose tissue therapy is a type of regenerative medicine known as orthobiologics. These are biological substances made from naturally occurring materials in the body, such as adipose tissue, a.k.a. body fat. Orthobiologics are used to aid in healing injured muscles, broken bones, and torn ligaments, among other things.
Adipose tissue is a rich source of mesenchymal stem cells found in bone marrow that are vital for creating and repairing skeletal tissues. These stem cells are believed to have analgesic, anti-inflammatory, anti-bacterial, and reparative properties that may play a critical role in healing.
Two recognized types of adipose tissue derivatives are stromal vascular function and micro-fragmented adipose tissue. These are named based on how the adipose tissue is processed. The latter involves washing the blood residues and pro-inflammatory oil without using separation centrifugation, additives, or enzymes. The harvested adipose tissue derivative is then passed through a size reduction filter to break the fatty tissue while preserving the microarchitecture mechanically.
Methods
The patient received a treatment called autologous micro-fragmented adipose tissue injection. Adipose tissue was taken from both upper buttocks and purified with a Lipogems kit. The micro-fragmented adipose tissue was then injected with an 18-gauge needle in a square pattern to fill the tissue defect under the skin.
There were four injection sites, with roughly 2 ml of micro-fragmented adipose tissue injected into each site, totaling 8 ml. After the procedure, the patient was advised to avoid submerging the affected area in water for 14 days, limit physical activity for four days, and to avoid taking NSAIDs.
The result
The patient experienced soreness around the injected areas on the first day. However, during the 4-week follow-up, he reported an overall improvement in his knee and no pain associated with the previously non-healing prosthesis-related ulcer. After returning to using his leg prosthesis, the patient resumed his physical activities without any restrictions.
This study presents the first known treatment of prosthesis-related residual limb ulcers using micro-fragmented adipose tissue therapy. Although the subject in this study showed significant improvement in just four weeks, further documentation and research are necessary, according to the researchers.